Patellar dislocation happens when the kneecap moves out of its usual position, often causing sharp pain and noticeable knee deformity In this post, we explore how to recognize the symptoms, understand the causes, and learn about the treatment options available for patellar dislocation.
Key Takeaways
- Early recognition of patellar dislocation symptoms, such as severe pain and swelling, is key for effective treatment and recovery.
- Treatment options for patellar dislocation may include conservative management for non-severe cases and surgical intervention for recurrent dislocations or fractures.
- Preventive strategies, including proper warm-up exercises and muscle strengthening, can be helpful for minimizing the risk of future patellar dislocations.
Recognizing a Patellar Dislocation
Identifying a patellar dislocation early is important for effective treatment and recovery. Key symptoms include severe pain, swelling, and a visible deformity of the knee. Patients often describe a sensation of the knee giving way, accompanied by an intense pain that can make it feel impossible to straighten the leg. This visible deformity occurs when the knee is bent and cannot be straightened, leaving the patella displaced from its normal position.
Immediate medical attention is necessary following a dislocated kneecap. Timely diagnosis and treatment may help reduce the risk of complications. The knee joint’s stability is compromised during a dislocation, resulting in an unstable kneecap that can lead to recurrent dislocations if not properly managed.
Recognizing symptoms and seeking timely medical intervention significantly improves the outcome of a patellar dislocation. Early diagnosis and treatment help reduce pain, swelling, and the risk of further dislocation.
Common Causes of Patellar Dislocation
Sudden impacts or missteps that leverage the body’s weight can cause traumatic patellar dislocations. Common scenarios include non-contact twisting injuries or direct blows to the knee, which are frequently seen in high-impact sports. Athletes are particularly vulnerable to these injuries, especially those involved in activities that require sudden changes in direction or jumping.
Genetic and congenital factors may predispose individuals to patellar dislocation. Congenital patellar dislocation is a rare condition where the patella does not develop properly within its groove, often linked to genetic factors that increase susceptibility. People with patellar instability, characterized by loose ligaments, are more prone to dislocations.
Anatomical and physiological factors can put certain populations at higher risk:
- Females may experience more lateral stress on their knees due to wider hips and looser ligaments.
- Teenagers are also particularly vulnerable, as their joints are more flexible during growth spurts.
- Larger individuals may face increased pressure on their joints, heightening the risk of dislocation.
Anatomy Relevant to Patellar Dislocation
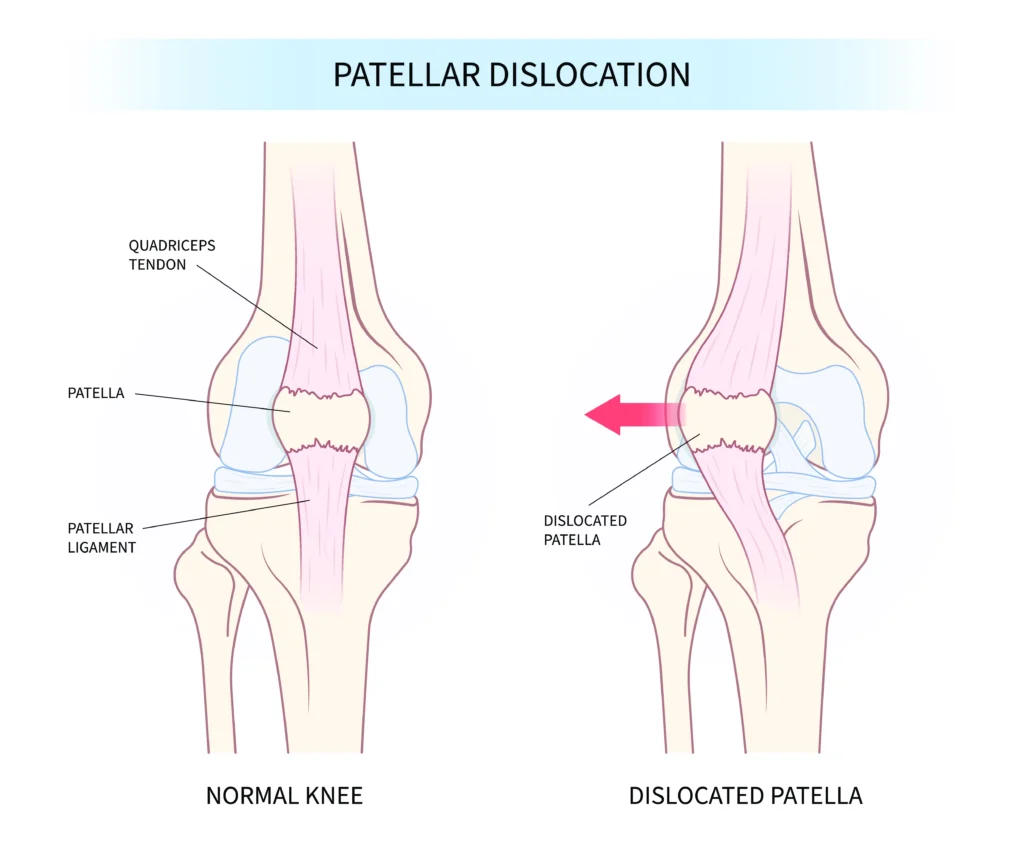
The knee joint is a complex joint that provides stability and allows for movement in the lower limb. Knowing the anatomical structures involved in patellar dislocation helps understand how the injury occurs. The medial patellofemoral ligament (MPFL) prevents lateral patellar dislocation. It acts as a restraint, keeping the patella aligned within the trochlear groove during knee motion.
The trochlear groove itself is designed to hold the patella in place, providing proper alignment as the knee flexes and extends. The quadriceps muscles, particularly the vastus medialis, play a key role in stabilizing the patella by controlling its position throughout a range of motion. When any of these structures are compromised, it can lead to patellar instability and increase the risk of dislocation.
Initial Diagnosis and Evaluation
Accurate diagnosis of a patellar dislocation is important for effective management and preventing future instability. The initial imaging approach frequently involves plain radiography, which is the most cost-effective method for evaluating patellar dislocations. MRI is particularly effective in diagnosing soft tissue injuries related to patellar dislocation, offering a detailed view of the damage.
Specific imaging views such as anteroposterior (AP), lateral, and sunrise views are helpful for a comprehensive evaluation of the dislocation. CT scans can offer improved sensitivity for detecting patellar tracking issues and measure the TT-TG distance, which is important in managing patellar dislocation.
Treatment Options for Acute Patellar Dislocation
Identifying the cause is important for developing an effective treatment strategy for acute patellar dislocation. Treatment options generally fall into two main categories: conservative management and surgical intervention. Each approach offers different benefits and is suitable for different situations based on the severity and recurrence of the dislocation.
Conservative management is often the initial treatment, especially for non-severe dislocations. Surgical treatment may be necessary for recurrent dislocations or when fractures are involved, to improve stability and prevent future incidents. An experienced knee specialist can assess the injury and help guide the most appropriate treatment approach.
Conservative Management
Non-surgical approaches can effectively manage acute patellar dislocations, especially when no loose fragments are present. Common non-surgical treatments include bracing and physiotherapy, focusing on strengthening the quadriceps, and core muscles. Rest, strengthening exercises, and using a patellar brace facilitate recovery, while gradual knee mobilization aids healing.
Specific knee braces can provide additional support during recovery and help maintain stability. These braces are particularly beneficial in the early stages of rehabilitation, helping to ensure proper alignment and reduce the risk of further dislocation.
Surgical Intervention
Surgical treatment might be needed for recurrent patellar dislocations to enhance stability and prevent future incidents. Fractures or recurrent episodes often necessitate surgical intervention, highlighting the need for tailored procedures based on the patient’s anatomical profile and predisposing factors.
Surgical procedures can include repairing or reconstructing the medial retinaculum to restore stability and proper alignment of the patella.
Rehabilitation and Recovery
Rehabilitation plays a role in recovering from a patellar dislocation. Recovery timelines vary, but many individuals begin to improve within several weeks to months following a first-time dislocation if no significant damage occurs. However, for those with recurring dislocations or severe injuries requiring surgery, recovery may extend beyond a year before they can return to sports. Rehabilitation timelines vary, with soft tissue procedures enabling earlier return to activity compared to bone procedures.
Key components of post-dislocation physical therapy include quadriceps strengthening, core strengthening, and proprioception exercises. Patients are encouraged to begin specific gait training early to avoid developing compensatory walking patterns. The RICE method (Rest, Ice, Compression, Elevation) can be helpful in early rehabilitation to reduce pain and swelling.
Specific braces can maintain stability during initial recovery, and functional tests like stair running and figure-of-eight tests assess readiness for athletic activities.
Preventing Future Dislocations
Preventive strategies may help minimize the risk of patellar dislocations and support long-term knee health. Appropriate protective gear during sports can safeguard the knee and reduce dislocation chances. Proper body mechanics during movement can decrease knee strain, reducing dislocation risk.
Incorporating preventive measures into daily activities and sports reduces the likelihood of initial and future dislocations. Maintaining strong and balanced muscles around the knee, along with being mindful of one’s body mechanics, can contribute to long-term stability and knee health.
Summary
In summary, patellar dislocation is a condition that requires prompt recognition, accurate diagnosis, and effective treatment to ensure optimal recovery and reduce the risk of future incidents. Understanding the causes, symptoms, and treatment options is important for managing this injury. Rehabilitation and preventive measures play a role in maintaining knee stability and long-term health.
By following the outlined strategies and seeking appropriate medical care, individuals can reduce the risk of recurrent dislocations and enjoy an active, healthy lifestyle. Remember, proper management and prevention are key to overcoming the challenges posed by patellar dislocations.
Frequently Asked Questions
What are the main symptoms of a patellar dislocation?
The main symptoms of a patellar dislocation are severe pain, swelling, and a noticeable deformity of the knee, often coupled with a feeling that the knee may give way.
What are common causes of patellar dislocation?
Patellar dislocation commonly results from sudden impacts, missteps, or twisting injuries, especially during high-impact sports. Additionally, genetic and congenital factors may increase susceptibility to this condition.
How is a patellar dislocation diagnosed?
A patellar dislocation is primarily diagnosed through plain radiography, which may be supplemented by MRI to assess any soft tissue injuries. Specific imaging views like anteroposterior, lateral, and sunrise are also utilized for a comprehensive evaluation.
What treatment options are available for patellar dislocation?
For patellar dislocation, conservative treatment options like bracing and physical therapy are available, but surgery may be necessary for recurrent dislocations or associated fractures.
How can future patellar dislocations be prevented?
To prevent future patellar dislocations, it is essential to use protective gear during sports, maintain proper body mechanics, and incorporate strengthening exercises for knee stability into your routine. These strategies collectively enhance knee support and reduce the risk of injury.